Meagan's Treatment
Meagan was treated for a type of brainstem tumor
called a Pontine
Glioma . Treatment options for this type of tumor were limited.
Because of its location, surgical options were unavailable and there
was no clearly beneficial chemotherapy regimen. On this page,
her treatments are listed in chronological order from diagnosis
to June 21, 2004.
Diagnosis
In January of 2003, Meagan showed signs which seemed
to indicate she had labyrinthitis, which is essentially an ear/sinus infection.
She had some trouble hearing and difficulty with her balance. Her pediatrician
recommended an antibiotic. When this didn't make a difference in her symptoms
and when her balance and ability to walk got considerably worse, he recommended
an MRI (Magnetic Resonance Imaging) brainscan. On Sunday February 23 we
had the MRI done first thing in the morning. The MRI took about an hour
and while it wasn't painful, the noise and strangeness of the process
were unsettling.
First thing in the morning on Monday February 24, a radiologist
looked at Meagan's films from the MRI. Unfortunately, the scans clearly
showed a malignant tumor on her pons, which is a part of the brain stem.
The tumor at that time was 5.5 centimeters tall, 5 centimeters deep, and
4.5 centimeters wide. The radiologist called her pediatrician at 9:35
in the morning. He immediately called us and began coordinating the process
of having Meagan admitted to the hospital for evaluation.
Hospitalization
Initially, we came into the pediatric emergency room.
Emma, Meagan's sister, stayed with a friend from school and her parents.
The three of us (Meagan, Jon, and Julie) were in shock. We met with a
team of doctors, including oncologists, radiologists, ER docs, and a stream
of residents. Fortunately, the University of Michigan has a separate pediatric
emergency room with private rooms for the more serious cases. Most of
that day was a blur, but we looked at films, talked to doctors, and set
up an intravenous line.
After initial consultations, Meagan was admitted to the
pediatric hematology/oncology ward. There, we met with even more doctors.
In the evening, her pediatrician visited us to check in. Julie Dybdahl,
who would become the family spokesperson in the following weeks, visited
with us. A pediatric oncologist explained some of the treatment options.
Meagan started the intravenous steroids that night. Julie picked up Emma
and Jon spent the night at the hospital. None of us got much sleep that
night.
On Tuesday, Meagan had visits from her friends Emma and
Kelsey. This buoyed her spirits on a very tough day. The girls played
card games and talked and with a long sleeved shirt over her IV hookup,
Meagan managed to mostly forget it was there. The parents talked about
next steps.
In the afternoon, she had a swallow test done. In this
test, a person swallows a variety of different foods and liquids. Each
substance is infused with barium and an x-ray video camera captures images
of the person swallowing. Unfortunately, the swallow test showed that
Meagan was unable to correctly swallow thin liquids. Each time she swallowed,
a small amount of liquid would be aspirated (breathed into her lungs).
For two weeks, she was unable to drink liquids such as water, juice, or
milk. Shortly before her birthday, she passed a subsequent swallow test
and was able to return to a full range of food and drink.
Tuesday afternoon, Meagan was released from the hospital
and we returned home.
Initial treatment
Meagan's initial treatment after diagnosis was high dose
steroids. The purpose of the steroids is to shrink the swelling surrounding
the tumor. The steroids may also have some limited effect in shrinking
the tumor itself. Her two day stay at the hospital included Decadron given
intravenously. Since then, she's been taking Decadron pills. Early on,
she had to take quite a lot of it, which resulted in joint aches, acne,
mood swings, and an enormous appetite. As the radiation treatments began
to work, she was able to reduce her steroid dose, which reduced these
symptoms.
Radiation treatment
Beginning in March, Meagan underwent six weeks of radiation treatment,
five days per week. On her first visit, Meagan had a fiberglass mask made.
It fit very tightly over her face and was solid mesh other than eye holes
and a mouth hole. When she went in for treatment, she lay face up on a
motorized table. The mask was placed over her face, then secured to the
table with wing nuts so that Meagan couldn't move her head. The table
was adjusted so that it was in exactly the same place for each treatment.
The radiation machine was not a tunnel like an MRI; instead it had a large
arm with a radiation head on it. The arm rotated to direct beams exactly
where they needed to go. The beams themselves were six convergent x-ray
beams. Two from each side and two from on top. Each beam was relatively
weak, but the point at which they crossed was very intense. Because of
the high radiation, Meagan needed to be by herself in the room during
the actual treatment. Technicians controlled the machine from an adjacent
room, monitoring her by closed circuit television.
During radiation treatments, Meagan had music playing,
a blanket, and a pillow which was signed by many of her friends. These
things helped her to focus on healing and make the treatments more tolerable.
Meagan reports that the radiation treatments didn't hurt, but felt like
a vibration. She had some spot hair loss where the beams entered and exited
but didn't lose a great deal of hair due to radiation.
Meagan responded very well to this treatment. She was
able to walk better, had less of a headache, and she had less double vision.
We were very heartened by these improvements.
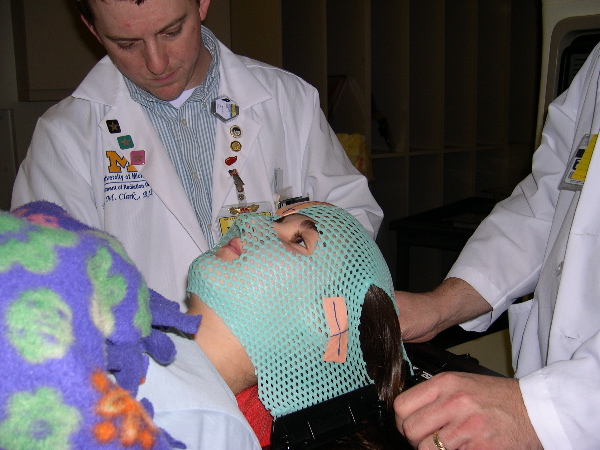 |
Meagan completed radiation treatments on April 22,
2003. This picture was taken on her last day of radiation. The mask
was used to properly align her head so that the radiation had the
maximum effect on the tumor and the minimum effect on other structures.
To celebrate completing radiation, Julie and the girls joined Jon
in Chicago. After daily appointments for six weeks, it was good
to have a few days without any appointments at all.
|
Complementary treatments
We also pursued several complementary treatments.
Meagan took multivitamins and antioxidants to combat the damage
to healthy tissue done by the radiation. To help fight the tumor, she
took Bromelaine and Maitake, along with cerebellum compus, a homeopathic
remedy, and a pill which is a mixture of grape leaves, strawberry leaves
and ant parts. She took a lot of pills.
Meagan visited a chi gung healer a few times a week,
which helped her to feel better and to have more energy. He also
recommended rotating her bed 90 degrees. Jon was skeptical, but it did
seem to help her sleep.
Meagan also took a homoeopathic preparation
of mistletoe
called Iscador. In Europe, this has been a common treatment for cancer
for several decades. We worked with Dr. Quentin McMullen at the Community
Supported Anthroposophical Medicine clinic for this treatment.
We found the visualization tapes
created by Belleruth
Naperstak to be helpful. Meagan uses visualization to help her relax
and concentrate on helping her body to heal.
Second MRI
On Tuesday, May 20 Meagan had her second MRI. The MRI
was at 6:30 in the morning. Meagan reported that it went much more smoothly
than the first MRI had. This was probably due to three factors: Meagan
felt better physically, knew what to expect, and had a nicer MRI technician.
Meagan had a shot of contrast dye to improve the quality of the scans
taken by the MRI. She then spent about 40 minutes inside the MRI tube,
getting pictures taken. Julie was just outside the tube, holding onto
Meagan's feet and giving her signals so that Meagan would know when the
pictures were being taken and she needed to be still.
At 10:00 the same morning, we met with Meagan's oncologist
to see the scans. While the MRI is inconclusive and open to interpretation,
there appeared to be quite a bit of improvement: The swelling around the
tumor was gone and the pons was smaller, indicating a reduction in tumor
size or possibly even that the tumor was gone. We had hoped that the MRI
would give us a more conclusive indication that the tumor was completely
eradicated, but still this was a very good result. Meagan's oncologist
says that the effectiveness of the radiation treatment was among the best
that she had seen.
Visit to Dana Farber Cancer Institute
On June 30, Meagan and Jon visited Dana Farber Cancer
Institute, which is affiliated with Harvard University and is located
in Boston. We sought a second opinion from the team there, hoping
that there would be treatments available there which were not available
in Michigan. Unfortunately, while there are experimental studies being
run, none of them seemed to be a clear advantage at this time. We
had hoped that a study would come along which would be of benefit.
As of July 2003 Meagan was
in very good shape so there we saw no immediate benefit in taking part
in the available studies.
September 2003 Update
Meagan and family had a wonderful summer 2003, filled
with travel, family, and all of the normal things people do. As of
late September 2003, Meagan had essentially none of the symptoms which
led to her diagnosis. She attended high school, rode her bike,
and was very much her usual self. We were grateful for the blessing
of this time together and hoped that it would last a long, long time.
Re-onset of symptoms
Unfortunately, Meagan began to have symptoms again in
January of 2004. At first, they were minor and we weren't sure if we were
really seeing symptoms again. But gradually it became clear that the headaches
and minor balance problems signaled the onset of recurring symptoms. On
January 30, we had a third MRI done. Analysis at the University of Michigan
hospital indicated probable tumor regrowth, with some chance that what
was seen on the MRI film was residual radiation damage.
In February and March, Meagan began taking an oral
chemotherapy drug, Temodar.
In conjunction with steroids and with the alternative medications
Meagan has been taking, her headaches went away. Other symptoms got
somewhat worse; these included difficulty walking, changes in vision,
and a gradual decline in the ability to use her right hand and leg.
Meagan was still going to school full time and her spirits were basically
good. We were deeply concerned by the recurrance of symptoms, but
kept uphope as best we could.
Second hospitalization
On Saturday March 27, Meagan had to be admitted to the
hospital for the first time since her initial diagnosis. She had been
fighting off a cold for a week, along with facing deteriorating symptoms.
On the 27th, her condition became worse, with a fever of over 102 and
a reduced ability to swallow. Fortunately, IV antibiotics and steroids
were able to get the fever under control and return some of her ability
to swallow. Meagan was hospitalized for four days, returning home after
meeting with an assortment of healthcare professionals. Her oral chemotherapy
regimen was changed from Temodar to VP 16. Meagan missed quite a bit of
school in the process of fighting off the cold and being in the hospital.
Friends, family, and lots of doctor and therapy visits kept her busy during
her time at the hospital.
Home again
Meagan was released from the hospital on March 31. The
month of April was a swirl of treatment visits from home health care nurses,
occupational and physical therapy, massage, art therapy, Reiki, and others.
Family and friends visited as well, supporting Meagan and keeping us all
occupied.
Meagan needed a walker or wheelchair to get around
and lost most use of her right hand and arm. That made many previously-routine
tasks a challenge. She was in school one or two periods per day and
got out of the house nearly every day. We found a new appreciation
for the importance of barrier free spaces.
Meagan took the oral chemo drugs VP16 and Tamoxifen,
along with the steroid Decadron to reduce swelling around the tumor
and Zantac for her stomach. It's a lot of pills.
Friends brought us meals, which was an enormous
help. The appointments and juggling work schedules for Jon and Julie
left little time to run the household.
Meagan's spirits were good for the most part. Spring was
here and the natural beauty around us was inspiring. It gave us hope.
May 28, 2004 update
Unfortunately, Meagan's condition continued to slowly
worsen. Her balance was worse than it was, with her right side weaker
and less usable. Double vision caused her to need to wear an eye
patch. Her speech was thicker and somewhat harder to understand. And
her swallowing, though still functional, became more difficult.
Meagan continued to take VP16, Tamoxifen, and Decadron. She began
taking Poly ICLC as soon as we received FDA clearance for her to
do so. Her tolerance of the chemo drugs was good, though she has
lost a certain amount of hair. We did not give up hope by any means,
though these were difficult times.
June 18: Third hospitalization
Meagan's condition continued to deteriorate in May and June.
While the chemo drugs she was taking didn't make her very sick, they didn't
seem to reverse the growth of the tumor, based on her worsening symptoms.
Heading into mid June, Meagan had increasing difficulty
swallowing. At first, she was okay as long as she didn't drink thin liquids.
But gradually the range of things she could swallow got less and less.
We began to discuss options such as a feeding tube to help her get nutrients
in the event that she lost the ability to swallow completely.
On June 18, Meagan began to have difficulty breathing. Her
lips turned blue and she was feeling pretty badly, so she was taken to
the hospital by ambulance. A chest x-ray in the emergency room indicated
fluid in her lungs. We decided as a family that we wanted to fight this,
so Meagan had a tube put in to suction the fluid and to help her breathe.
She was admitted to the intensive care unit so that she could continue
to have a breathing machine as she continued to fight the pneumonia and
possible infection. By the morning of June 19, her fever was reduced,
her blood pressure (which had been low) was relatively normal, and a chest
x ray indicated that her lungs had cleared quite a bit.
In the afternoon of June 19, Meagan was able to communicate
a little through finger spelling. The first thing she wanted to know was
what time it was, as she had been sedated since the previous afternoon.
The next thing she spelled out was B-O-R-E-D. It was a big relief to have
her be comfortable enough that boredom was the problem she wanted to communicate.
As of June 19, our hope was to get rid of the pneumonia
which brought Meagan to the hospital, figure out how to keep it from
recurring, and get her home again. It wasunclear how long that would
take to accomplish, but we had hoped it would be only be a couple of
days.
Unfortunately, on June 20 it became clear that Meagan
would not be able to breathe without a ventilator. The tumor had taken
too much of her ability to draw an effective breath. This was an unexpected,
very serious setback. Realizing that she would not be able to go home
or even to leave the intensive care unit, Meagan began to prepare
herself for turning the ventilator off, which she realized would result
in her death. We talked (through fingerspelling) about what kind of
service she would like to have and we hurriedly arranged for a few
visitors.
On the afternoon of June 21, the ventilator was turned off.
Meagan lost consciousness very quickly. Her body struggled to go on for
a few hours, but it was clear that she was gone. At 8:35 in the evening,
Meagan passed from this life.
At some point, I may be able to write more about her final
days, but for now this page will not be updated further. Please see the
services page for information about her burial
and memorial service.
Last updated July 7, 2004.
|


